Outline and contents of the didactic unit
Sexual and asexual reproduction
Years and years of observations and studies about the organism that populate Earth led us to state that some of them reproduce by generating one or more new organisms identical to them selves, while for others reproduction involves more than one individual and the new generated organism shares only part of his genetic inheritance with each of the parents, being a new combination of some of the genes of them both. We also observed organisms of certain species able to use either of the two strategies depending on the situation. What are the advantages and disadvantages of each of these strategies through evolution? The question has puzzled the Biologists for a long time and has led to many interesting studies. We rest insured though that each of the described strategies has worked well for the organisms that have used it for a long time and that none of the strategies turned out to be the most advantageous for everyone. 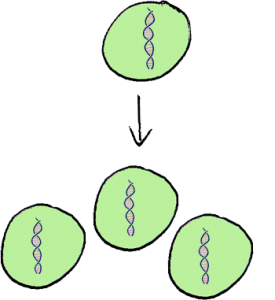
When an individual reproduces by generating organisms identical to himself, we call it asexual reproduction.
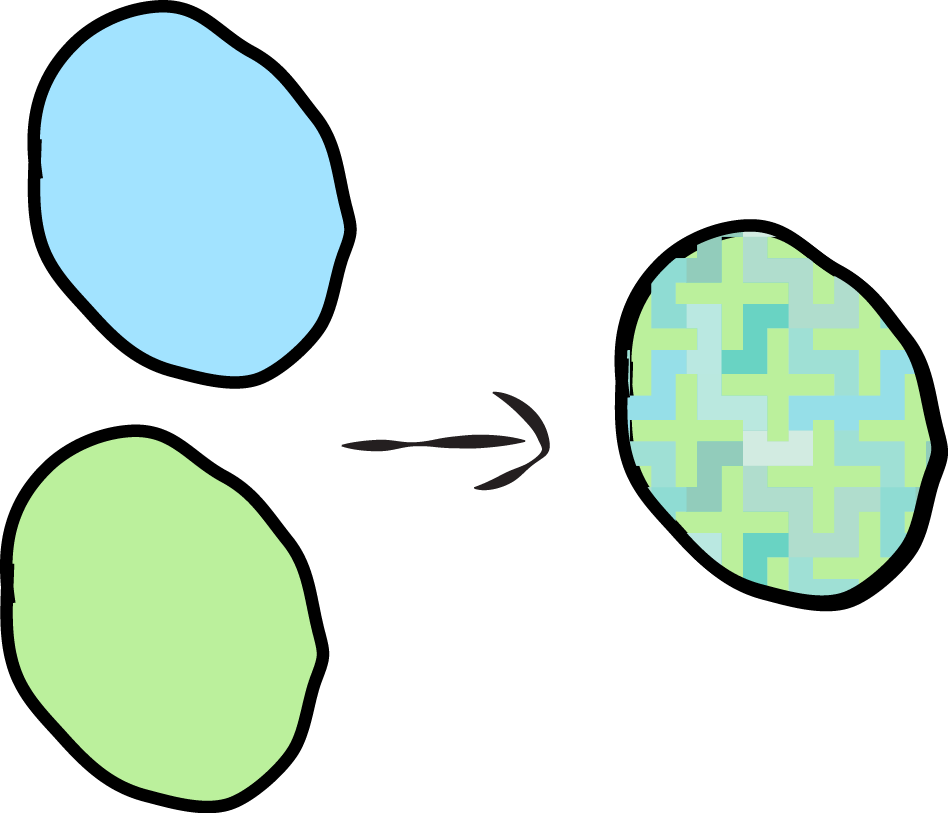 When reproduction involves more than one organism and implies the mixing of their genetic material in the newborn, we talk of sexual reproduction.
When reproduction involves more than one organism and implies the mixing of their genetic material in the newborn, we talk of sexual reproduction.
For those of you who wander what could be the advantage of using sexual or asexual reproduction for each of the different species that we have studied so far and for mankind in particular, I suggest to read a very nice book written by Andrea Pilastro entitled “Sesso ed evoluzione” available in Italian or to read this much shorter article on line “the paradox of sexual reproduction“.
Meanwhile it is important for the all of us to have a good working definition of sexual and asexual reproduction and to look at a few examples in nature of each of the two strategies. A synthetic and useful source of information is provided by the University of Utah at the following link: https://learn.genetics.utah.edu/content/basics/reproduction/ Read the definition and then click on each of the figures to learn about the reproductive strategy of the species represented and test your comprehension by taking the multiple choice quiz.
At the base of cell reproduction is mitosis. The two daughter cells have the exact same genetic information of the mother cell.
A special type of cell division, called meiosis, is instead associated to sexual reproduction. After meiotic division the daughter cells bear half of the genetic information of the mother cell. If the mother cell is diploid, the daughter cells will be haploid. Haploid cells do not perform meiosis, while polyploid cells do. Meiosis is the type of cell division performed by unicellular organisms for sexual reproduction and is also the cell division used for the production of the cells of the germinal line in pluricellular organisms that reproduce sexually. You already studied cell division and it is important that you remember it in order to understand reproduction.
Functional attributes of sexual reproduction
- Organisms that reproduce sexually switch though their lifecycle between an haploid (n chromosomes) and a diploid (2n chromosomes) state.
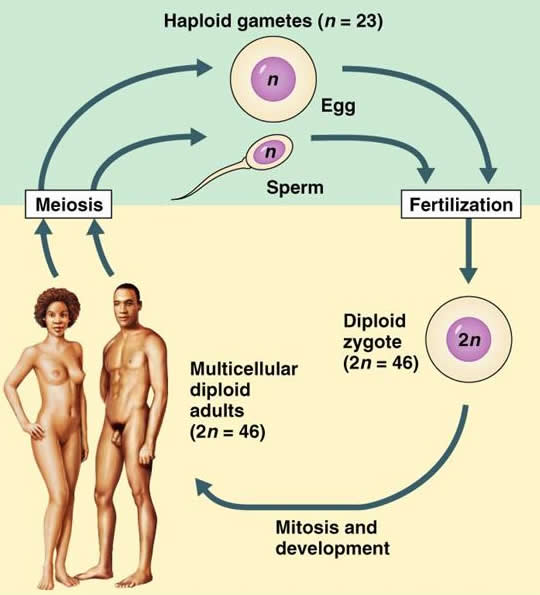 In humans the haploid state is represented by the cells of the germinal line, that will give rise to the new diploid individual after fertilisation. The human individual is diploid.
In humans the haploid state is represented by the cells of the germinal line, that will give rise to the new diploid individual after fertilisation. The human individual is diploid.
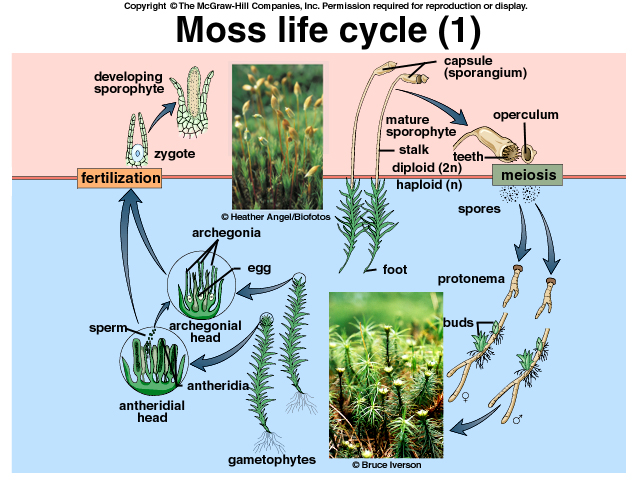 Moss instead, for example, spends the majority of his lifetime as a haploid gamete, it becomes diploid for a brief time after fertilisation and the diploid individual undergoes very soon the meiosis and releases the new haploid organism.
Moss instead, for example, spends the majority of his lifetime as a haploid gamete, it becomes diploid for a brief time after fertilisation and the diploid individual undergoes very soon the meiosis and releases the new haploid organism.
Some plants are polyploid (a*n chromosomes), they will switch between a*n chromosomes and 2a*n chromosomes. The haploid or a*nploid cells involved in sexual reproduction are called gametes.
- During sexual reproduction two cells with half of the genetic material necessary to form a new individual (the gametes) fuse together. The two gametes belong to two different sex types. We call “female” the cells that bear both the DNA and the cytoplasm for the new individual; “male” the cells who contribute to the new individual mainly with their DNA. The female gametes are called ova or egg cells, the male gametes are called sperms.
- In pluricellular organism there is an apparatus who produces the gametes and also a system to ensure that the gametes of the two different cell types will come in contact with each other. In the next session we will study how the human gametes are produced and how are body ensures that the two different type of gametes meet with each other and fuse.
Generation of male and female gametes in H. sapiens
The production of egg cells in the human female
The primordial follicles are cells found inside the ovaries and they are formed during the embryogenic development. The oogenesis (literally the formation of the ovum) begins in the human females before or shortly after birth, when the primordial follicles develop into primary oocytes. This process has never been observed in any adult human female and it is therefore believed that the number of oocytes produced at this early stage is also the total number of oocytes that that female is going to have during her lifetime.
The primary oocytes start their cell cycle and then freeze at the stage of profase I, when they are ready to perform the first meiotic division, but they are not doing it yet. During the first stages of the cell cycle these cells grow and accumulate ribosomes, RNA and energetic molecules.
Puberty sets the beginning of a new developing stage of the oocytes towards the formation of ova or egg cells. With the onset of puberty, one primary oocyte at a time comes to maturation following a precise hormonal cycle. The maturation consist in the first meiotic division of the primary oocyte that generates two haploid cells: a secondary oocyte and polar body. The two cells have each half of the genetic information of the primary oocyte. However one of them, the secondary oocyte, also inherits the cytoplasm, whilst the polar body bears a very little amount of cytoplasm and rapidly degenerate and dyes. This division implicates sources of genetic variation, such as random inclusion of either parental chromosomes, and chromosomal crossover, to increase the genetic variability of the gamete.
Immediately after meiosis I, the haploid secondary oocyte initiates the second meiotic division. However, once again, the process is halted before completing the division. The secondary oocyte sites in the uterus for at least 72 hours ready to be fertilised.
If fecundation doesn’t occur, the oocyte is discarded at this immature state during the menstrual cycle.
Should fertilisation occur the oocyte completes the second meiotic division before allowing the fusion of its nucleus with the one of the sperm. In this case again the division is asymmetric and generates an ootid (the mature ovum) and another polar body.
With the ongoing of menopause the majority of the primary oocytes have undergone their maturation process. A few of them my occasionally come to maturation during menopause but the all cyclic process has substantially come to an end.
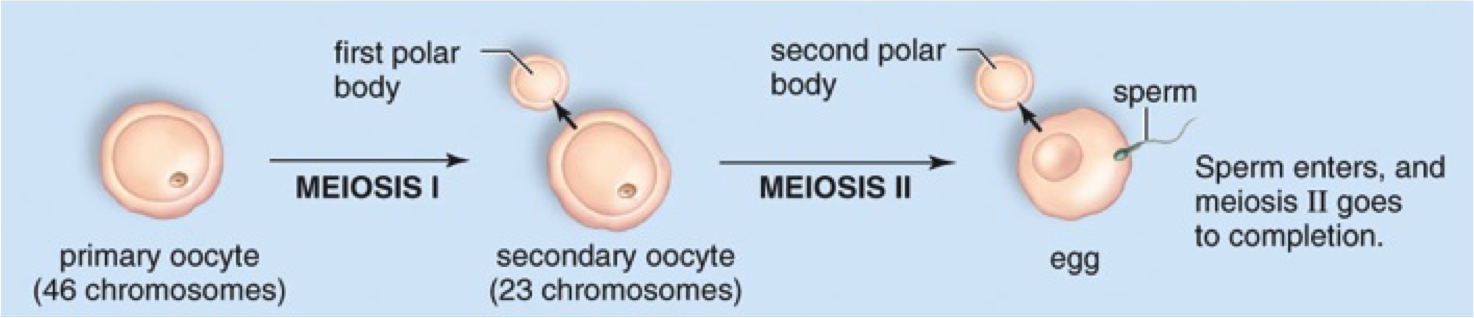
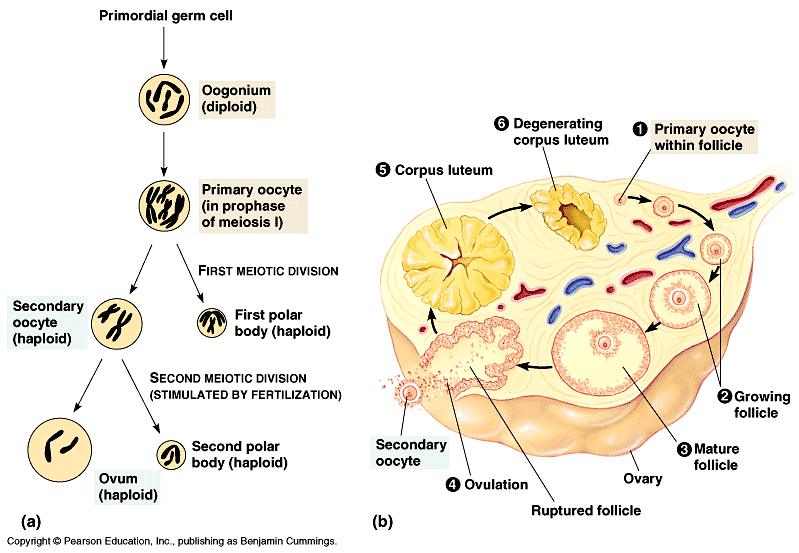
The production of sperm in the human male
Primordial germ line cells are formed in the male individual during embryonic development.
With the onset of puberty a process called “spermatogenesis” begins. It is the process in which spermatozoa are produced from the male primordial germ cells.
Spermatocytogenesis is the cellular process that results in the formation of spermatocytes possessing half the normal complement of genetic material. In spermatocytogenesis, a diploid spermatogonium, which resides in the basal compartment of the seminiferous tubules, divides mitotically, producing two diploid intermediate cells called primary spermatocytes. Not all the spermatogonia mature into spermatocytes, some just divide mitotically to produce copies of themselves, ensuring that the supply of spermatogonia doesn’t run out during life.
Each primary spermatocyte then duplicates its DNA and subsequently undergoes meiosis I to produce two haploid secondary spermatocytes, which will later divide once more into haploid spermatids. This division implicates sources of genetic variation, such as random inclusion of either parental chromosomes, and chromosomal crossover, to increase the genetic variability of the gamete.
Each cell division from a spermatogonium to a spermatid is incomplete; the cells remain connected to one another by bridges of cytoplasm to allow synchronous development.
The now mature spermatids begin to form a tail and to condense their DNA and become spermatozoa. At the anterior part of the tail we find mitochondria to ensure energy supply. This final maturation takes place under the influence of testosterone.
This process that starts at puberty, usually continues uninterrupted until death, although a slight decrease can be discerned in the quantity of produced sperm with increase in age.
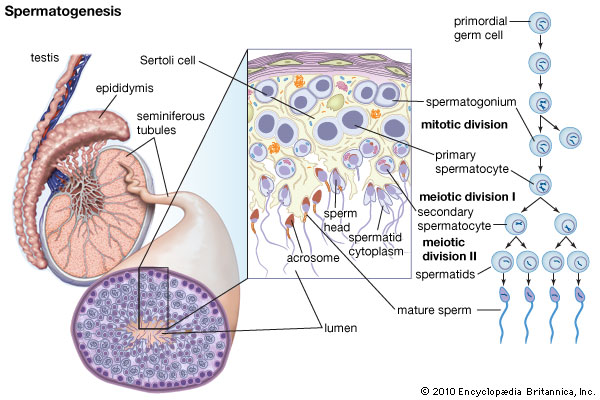
Anatomy: the system that generates and delivers the gametes
Two sex types, two gametes types, many genders
As we discussed in one of the previous paragraphs, in order to generate an offspring through sexual reproduction we need to have two different gametes, each one from a different sexual type. If something goes wrong in the maturation of the gametes, fertilisation does not occur.
The gametes are produced by complex systems of tissue and organs that develop during the growth and development of the human body. Moreover an external sexual apparatus is needed so that the gametes of the two different sex types come in contact. Finally the individuals bearing the two different gametes have to recognise each other and to desire making a contact and allowing their gametes to mate. The internal and external apparatus and all the secondary sexual characters are coded by a number of different genes and require to develop a number of processes that happen at various stages of our life. By reading together a recent review published on the scientific journal Nature we found out that we do not have two clearly distinct genders in humans, but a number of different combination of sexual characteristics, many of them leading to fertile individuals. It is also interesting to read about sex verification in sports throughout the history of female sport competition in a recent review article.
While the sex types in human are two, while the type of gametes are again two (eggs and sperms), the type of people carrying the gametes are many, with a different mixture of sexual characteristics. And this is how the human body has routinely worked throughout evolution.
As male and female individuals develop from zygotes into fetuses, into infants, children, adolescents, and eventually into adults, sex and gender differences at many levels develop: genes, chromosomes, gonads, hormones, anatomy, and psyche.
Sex differences range greatly and include physiologically differentiating. Sex-dichotomous differences are developments which are wholly characteristic of one sex only. Examples of sex-dichotomous differences include aspects of the sex-specific genital organs such as ovaries, a uterus or a phallic urethra. In contrast, sex-dimorphic differences are matters of degree (e.g., size of phallus). Some of these (e.g., stature, behaviors) are mainly statistical, with much overlap between male and female populations. Nevertheless, even the sex-dichotomous differences are not absolute in the human population, and there are individuals who are exceptions (e.g., males with a uterus, or females with an XY karyotype), or who exhibit biological and/or behavioral characteristics of both sexes.
Sex differences may be induced by specific genes, by hormones, by anatomy, or by social learning. Some of the differences are entirely physical (e.g., presence of a uterus) and some differences are just as obviously purely a matter of social learning and custom (e.g., relative hair length). Many differences, though, such as gender identity, appear to be influenced by both biological and social factors (“nature” and “nurture”).
Apparatuses
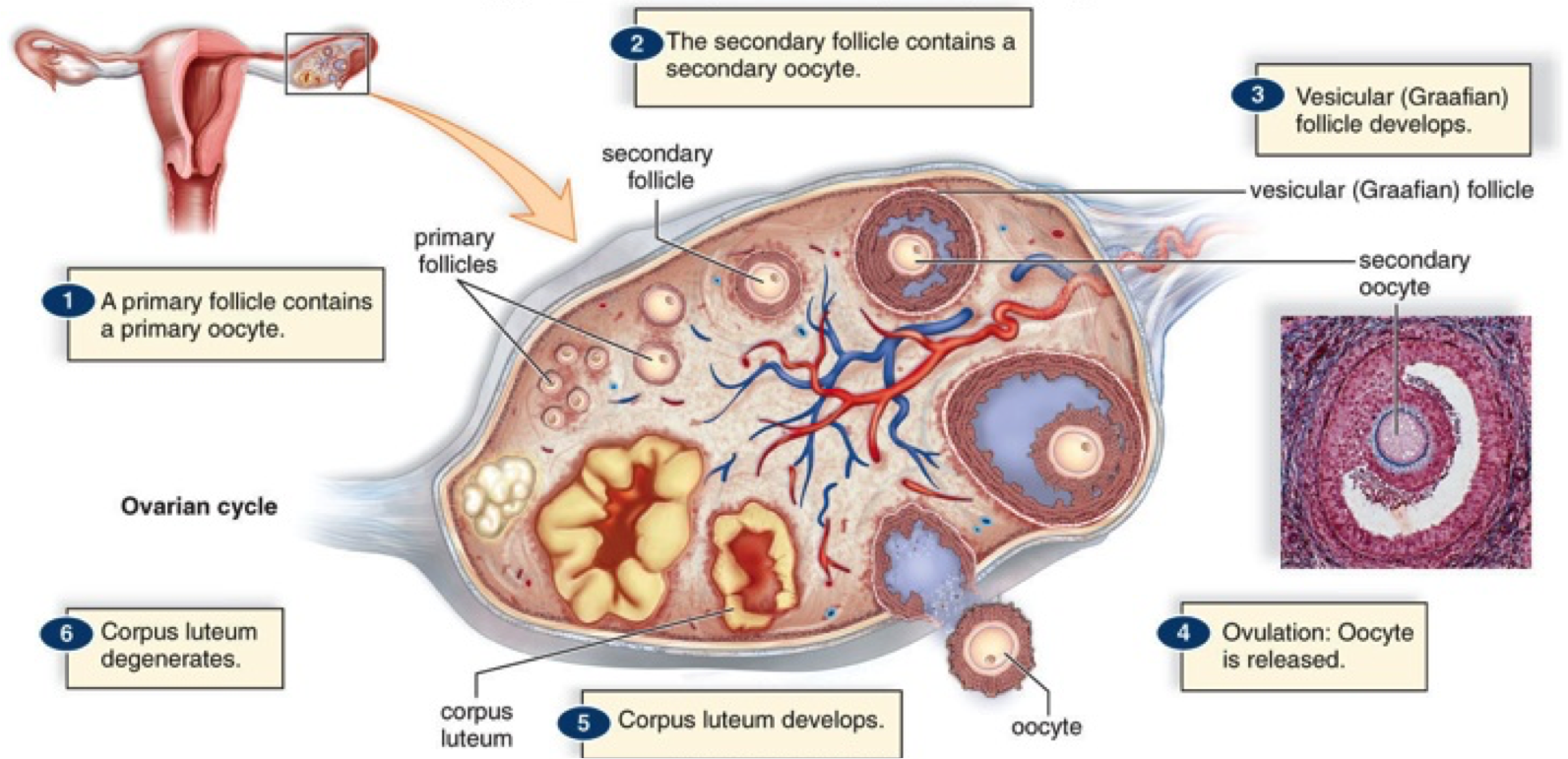
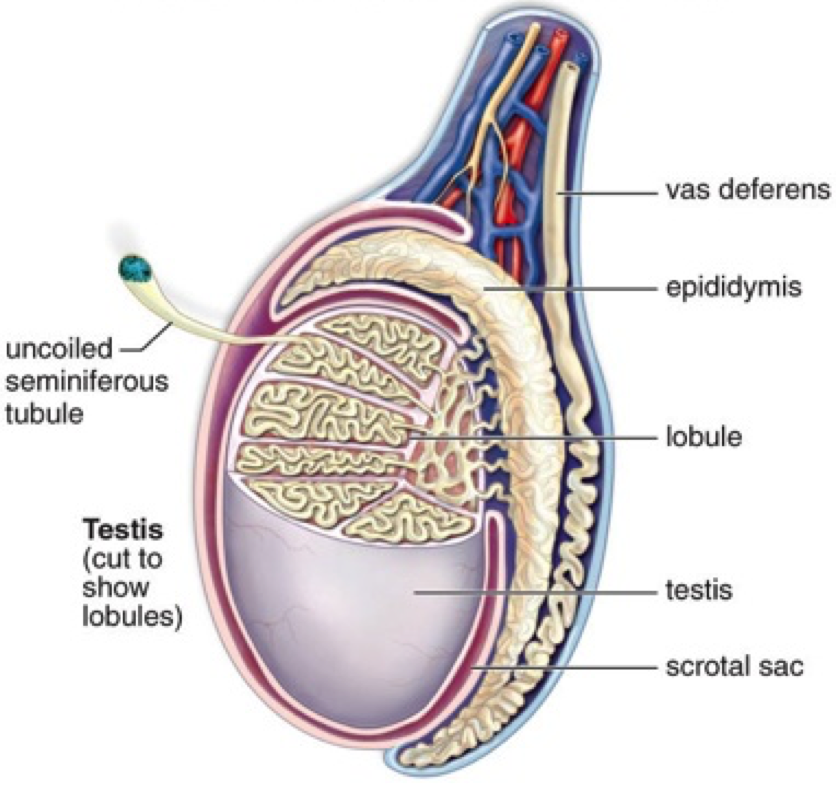
The hormones involved in the development and functioning of the reproductive apparatus
Early determination
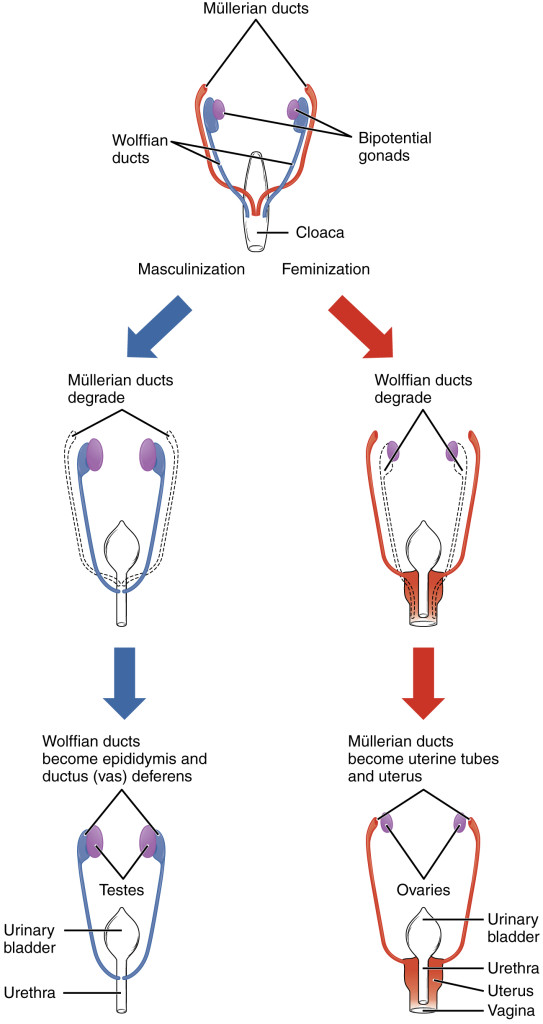
Image by OpenStax College – Anatomy & Physiology, Connexions Web site, shared under CreativeCommons3 licence
A fascinating aspect of development is the potential of sexually undifferentiated embryos to generate male or female individuals. The initial stages of gonadal and genital development of male and female embryos are indistinguishable by morphological criteria. In females, ducts give rise to uterus, fallopian tubes, and proximal vagina, while in males, ducts develop into multiple reproductive organs including vas deferens, seminal vesicles, and epididymis.
Humans have forty-six chromosomes, including two sex chromosomes, XX in females and XY in males. It is obvious that the Y chromosome must carry at least one essential gene which determines testicular formation. A gene in the sex-determining region of the short arm of the Y, now referred to as SRY, has been found to direct production of a protein, testis determining factor, which binds to DNA, inducing differentiation of cells derived from the genital ridges into testes. In transgenic XX mice (and some human XX males), SRY alone is sufficient to induce male differentiation.
An experiment performed at the end of the ’40 by Jost (Jost 1947; Jost 1953) demonstrated that in mammals female differentiation occurs irrespective of the genetic sex in the absence of testicular hormones. As we saw (Nature 2015) the female determination also depends on a number of genes and early hormonal signals, nevertheless the presence of the SRY gene is necessary for the genetic determination of males.
Childhood
Sexual dimorphism of skeletal structure develops during childhood, and becomes more pronounced at adolescence. Sexual orientation has been demonstrated to correlate with skeletal characters that become dimorphic during early childhood (such as arm length to stature ratio) but not with characters that become dimorphic during puberty—such as shoulder width.
Puberty and adult age
As mentioned earlier there is a number of our characteristics associated to sex. The all of them either appear for the first time or undergo important changes at the onset of puberty.
What is so special about puberty? During childhood the levels of hormones secreted by the hypothalamus and by the adenohypophysis steadily increase, until they reach a concentration which is enough for the gonads to perceive the message and respond. This critical point is reached at puberty. While the hypothalamus constantly receives stimuluses from various parts of our body that induce the secretion of hormons, the gonads, upon reception of the hormonal message, act to inhibit the secretion. This system of communication keeps the concentration of the hormones stable throughout adult life.
The hypothalamus is located in the brain and secretes GnRH. GnRH binds to receptors on the secretory cells of the adenohypophysis. In response to GnRH stimulation, the secretory cells of adenohypophysis produce LH and FSH, which travel into the blood stream. These two hormones communicate to the gonads.
In males, LH binds to the interstitial cells, causing them to secrete testosterone. Testosterone is required for normal spermatogenesis, is responsible for the appearance and maintenance of secondary sexual characteristics, and inhibits the hypothalamus. FSH binds to spermatogenic cells, which also respond by secreting a protein that finally has the effect of inhibiting the hypothalamus.
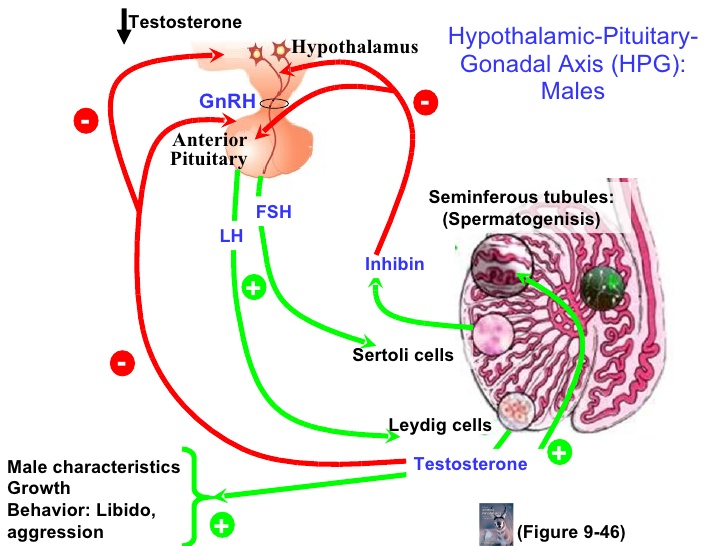
In females FSH acts on the ovaries, that are in direct contact with the forming oocyte. The granulosa cells in the ovaries secrete inhibin that inhibits the release of FSH. LH acts on the cells which are not in direct contact with the developing germ cells. These cells respond by promoting the secretion of oestrogen, and at times progesterone, that in most cases produce a negative feedback onto the pituitary and the hypothalamus to decrease FSH and LH production. Oestrogen and progesterone also have an effect on the uterus, they stimulate the thickening of the endometrium, and on the secondary sex characteristics of female.
The LH and FSH that reach the ovary induce the follicles to start the maturation process. In response we observe a secretion of oestrogen from the follicular area. The oestrogen acts by inhibiting the secretion of LH and FSH by the hypothalamus, by signalling to the uterus to thicken the endometrium and by activating the expression of genes associated to female secondary sex characteristics. The quickest follicle to mature continues its maturation and produces a big amount of oestrogen fairly quickly. This boost of oestrogen causes an increase in GnRH production and as a consequence an increase in FSH and LH production. This increase in LH, called the LH surge, stimulates ovulation. After ovulation the cells of the follicle produce oestrogen and also progesterone for about two weeks. If in these two weeks the ovule hasn’t been fertilised the follicular cells degenerate and the all process has to start all over again. When the follicular cell degenerate they stop producing hormones, the amount of oestrogen and progesterone dramatically decrease, the uterus no longer receives the hormonal signalling and we have the menstruation.
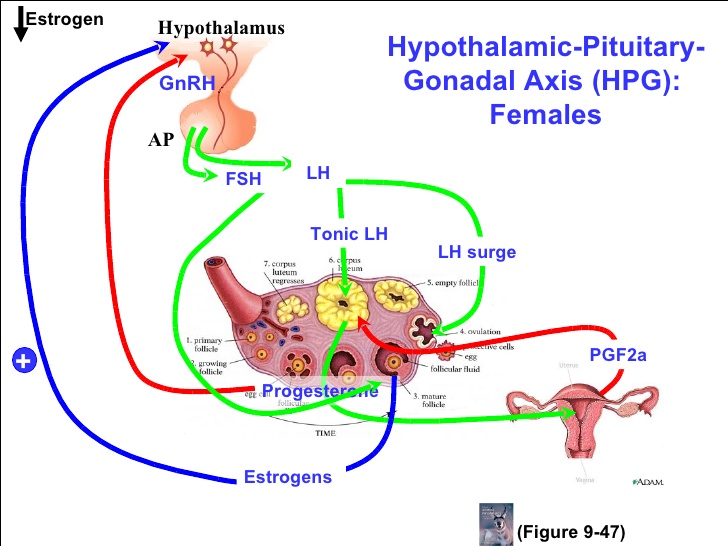
Review and check out your knowledge about sexual hormones at the following links: hormons and puberty, hormones and the menstrual cycle
Diseases associated with the sexual apparatus
Sexually transmitted diseases
Sexually transmitted diseases (STDs) are infections that are commonly spread by sex. The causes of STDs are bacteria, parasites and viruses. There are more than 20 types of STDs, including
Most STDs affect both men and women.While STD caused by bacteria or parasites can be treat with antibiotics or other medicines (syphilis, gonorrhea, chlamydia, trichomoniasis), STD caused by viruses (herpes, hepatitis B, HIV/AIDS, and HPV) cannot be cured, sometimes though, medicines can keep the viral disease under control. In addition, some organisms responsible for bacterial infections can develop resistance to certain antibiotics (it is the case of gonorrhea). Correct usage of latex condoms greatly reduces the risk of catching or spreading STDs. Vaccination is also an effective prevention for some STDs (e.g. hepatitis; HPV).
We discussed during our classes the reasons why the fluids exchanged during sexual intercourse are ideal vehicles for parasites to survive and spread.
For further information and curiosities about the various diseases, symptoms and cures you can find information from a very reliable source: the page of the “US National Library of Medicine” on this topic.
Diseases of the sexual apparatus
Penis disorders. Problems with the penis can cause pain and affect a man’s sexual function and fertility. Penis disorders include
- Erectile dysfunction – inability to get or keep an erection
- Priapism – a painful erection that does not go away
- Peyronie’s disease – bending of the penis during an erection due to a hard lump called a plaque
- Balanitis – inflammation of the skin covering the head of the penis, most often in men and boys who have not been circumcised
- Penile cancer – a rare form of cancer, highly curable when caught early
Testicular disorders. Testicles, or testes, make male hormones and sperm. They are two egg-shaped organs inside the scrotum. It’s easy to injure your testicles because they are not protected by bones or muscles. Men and boys should wear athletic supporters when they play sports. You should examine your testicles monthly and seek medical attention for lumps, redness, pain or other changes. Testicles can get inflamed or infected. They can also develop cancer. Testicular cancer is rare and highly treatable. It usually happens between the ages of 15 and 40.
Benign Prostatic Hypertrophy. The prostate is a gland in men. It helps make semen, the fluid that contains sperm. The prostate surrounds the tube that carries urine out of the body. As men age, their prostate grows bigger. If it gets too large, it can cause problems. An enlarged prostate is also called benign prostatic hyperplasia (BPH). Most men will get BPH as they get older. Symptoms often start after age 50. BPH is not cancer, and it does not seem to increase your chance of getting prostate cancer. But the early symptoms are the same.
Breast cancer affects one in eight women during their lives.Men can have breast cancer, too, but the number of cases is small. Breast self-exam and mammography can help find breast cancer early when it is most treatable. Treatment may consist of radiation, lumpectomy, mastectomy, chemotherapy and hormone therapy.
Cervical cancer. The cervix is the lower part of the uterus, the place where a baby grows during pregnancy. Cervical cancer is caused by a virus called HPV. The virus spreads through sexual contact. Most women’s bodies are able to fight HPV infection. But sometimes the virus leads to cancer. By getting regular screenings, you can find and treat any problems before they turn into cancer. Treatment may include surgery, radiation therapy, chemotherapy, or a combination. The choice of treatment depends on the size of the tumor, whether the cancer has spread and whether you would like to become pregnant someday. Vaccines can protect against several types of HPV, including some that can cause cancer (tutte le informazioni utili su http://www.fondazioneveronesi.it/articoli/ginecologia/tumore-della-cervice-uterina-e-vaccino-hpv-attenzione-alle-bufale/)
Birth control
Maturation of the gametes
Hormonal birth control administration in female: hormonal birth control is effective because it works by mimicking the phase of the female’s cycle when the ovulation has already taken place. The primary active ingredients are synthetic progesterones, which mimic biologically derived progesterone (look up in the above text and interactive figures when the progesterone is secreted). The synthetic progesterone prevents the hypothalamus from releasing GnRH and the pituitary from releasing LH and FSH; therefore it prevents the ovarian cycle from entering the ovulation phase and prevents follicle development and ovulation. It does not interfere with the uterine cycle, which responds to mild concentration of oestrogen and progesterone secreted by the follicles. These hormones indeed are still secreted regularly. Menstruation therefore regularly occurs, while ovulation doesn’t. Administration of this treatment can be achieved via: birth control pills, patches, shots, vaginal rings.
Delivery of the gametes
Avoiding sexual intercourse between fertile people of opposite sex.
Condoms, female condoms and cervical caps prevent the encounter of the gametes by preventing the exchange of sexual fluids which are kept separate by an impermeable barrier.
A vasectomy is a procedure to cause permanent sterility in a man by preventing the transport of sperm out of the testes. A small incision is made in the scrotum and each vas deferens is tied off and cut apart preventing sperm from being released within the ejaculate. The small skin incision is stitched closed and the surgery does not affect a man’s sexual function.
Tubal ligation is a permanent form of birth control. The surgery closes the fallopian tubes, which connect the ovaries to the uterus. Women can return to most normal activities within a few days. Tubal ligation can sometimes be reversed, but not always.
Implantation of the embryo into the uterus
Intrauterine devices (IUDs) are inserted into the uterus through the cervix, and they prevent normal implantation of the developing embryonic mass within the endometrium. Some early IUD designs produced serious side effects such as perforation of the uterus, and, as a result, many IUDs have been removed from the market. However, data indicate that IUDs are effective in preventing pregnancy.
RU486, blocks the action of progresterone, causing the endometrium of the uterus to slough off as it does at the time of menstruation. Therefore it can be used to induce menstruation and reduce the possibility of implantation when sexual intercourse has occurred near the time of ovulation. It can also be used to terminate pregnancies.
Assisted reproductive technology
Assisted reproductive technology (ART) is used to treat infertility. It includes fertility treatments that handle both a woman’s egg and a man’s sperm. It works by removing eggs from a woman’s body. The eggs are then mixed with sperm to make embryos. The embryos are then put back in the woman’s body. In vitro fertilisation (IVF) is the most common and effective type of ART. ART procedures sometimes use donor eggs, donor sperm, or previously frozen embryos. It may also involve a surrogate or gestational carrier. A surrogate is a woman who becomes pregnant with sperm from the male partner of the couple. A gestational carrier becomes pregnant with an egg from the female partner and the sperm from the male partner. The most common complication of ART is a multiple pregnancy. It can be prevented or minimised by limiting the number of embryos that are put into the woman’s body, but this has been a subject of ethic discussion.
What are my objectives while studying this unit
- being able to define sexual and asexual reproduction and to associate each reproductive process with the type of cell division process involved in it; keeping in mind at least a few examples in nature of each of the processes that I describe (i.e. mitosis goes on in the somatic cells of our body during growth and development; germinal line cells are produced by meiosis; H. sapiens reproduces sexually; Sequoia can reproduce both sexually and asexually.. and so on..)
- understanding the principal attributes of sexual reproduction, being able to tell them and to provide examples and explanations
- knowing the processes of male and female gametogenesis in human; being able to make comparison between them; being able to correlate these processes with possible causes of infertility and possible strategies of birth control
- knowing the secondary sex characteristics of adult humans (reference to study); knowing the main genes and processes associated with the development of the sexual apparatuses and the sexual characteristics of humans (reference to study)
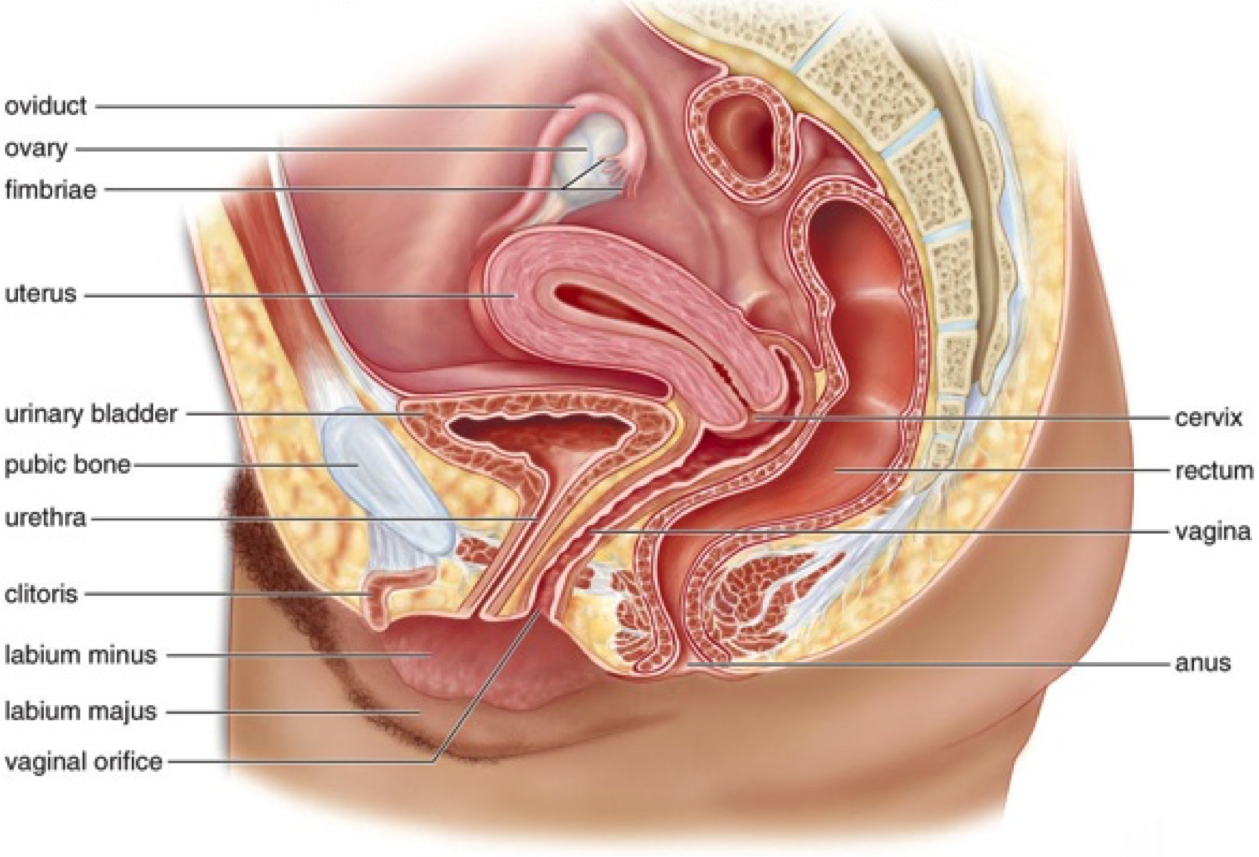
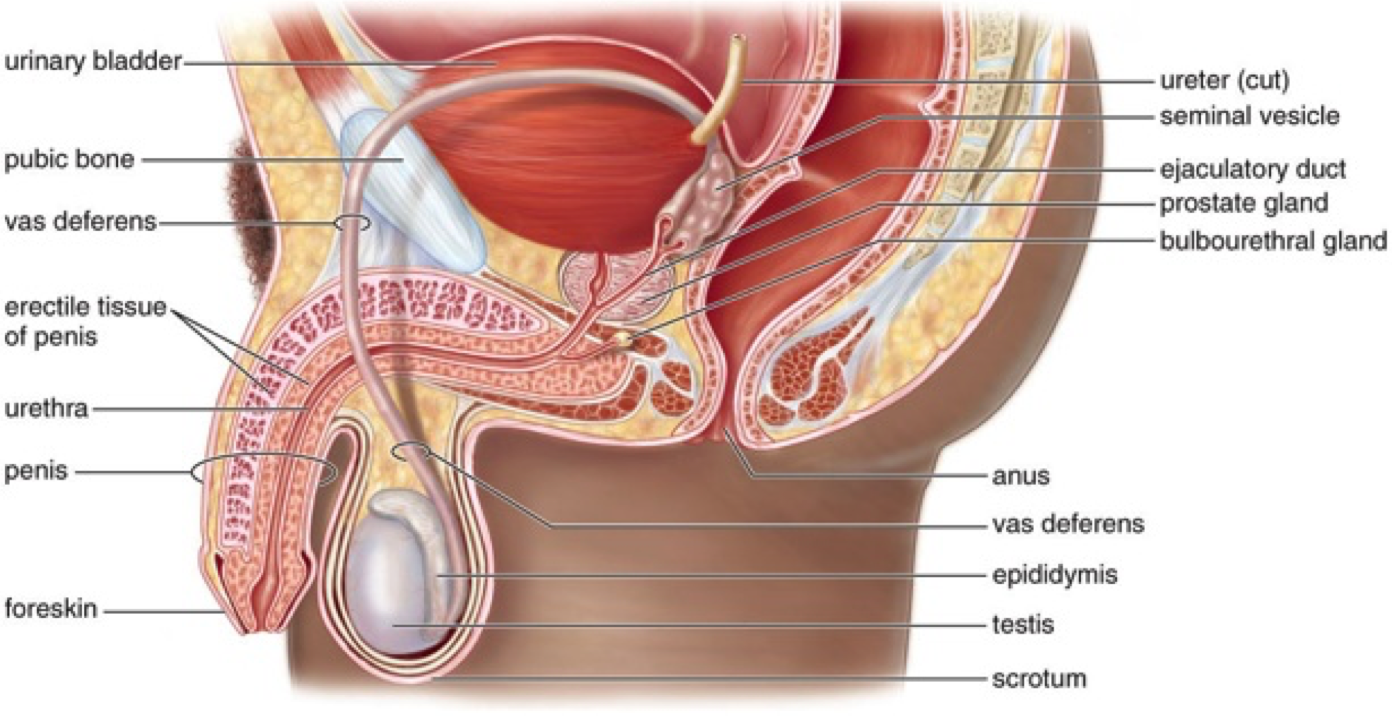
- being able to describe the main anatomic characteristics of male and female genitalia and to recognise them on a picture
- knowing the main steps of sexual development
- understanding the flux of communication in the pituitary-hypothalamus-gonad axis in male and female; being able to make comparisons between the male and female hormonal signalling; understanding the connection between the ovarian and the uterine cycle
- being aware of sexually transmittable diseases and means to control or prevent their transmission; being aware of the most common and harmful diseases that affect the sexual apparatuses and the relative cures and prevention
- understanding the mechanisms of birth control procedures
A few sources of information for the above contents which aren’t explicitly referred to in the text
- English version of Wikipedia and in particular the following entries: spermatogenesis; oogenesis; sexual differentiation; HPG axis; sexually transmitted infections
- “Hormones in male sexual development” 2000 Genes & Development Vol 14 pag 3075-3086. doi:10.1101/gad.843800
- Duke University – Lectures of Physiology at coursera.org
- MedLine Plus








Ragazzi come sta andando lo studio? Scrivetemi pure nei commenti se c’è qualcosa che non è chiaro o che vi sembra difficile.. il compito sarà fra poco..
Salve prof! Sono Roberto masetti 4A. Non riesco ad aprire il primo link del paragrafo “puberty and adult age”, c’è scritto che il sito è stato archiviato.
a me funziona..
Salve prof! Sono Roberto masetti 4A. Non riesco ad aprire il primo link del paragrafo “puberty and adult age”, c’è scritto che il sito è stato archiviato.grazie!
Salve prof
Precisamente quello che ci sarà nel compito è:
“Struttura” maschile e femminile con i termini da completare
La formazione dello sperma e della cellula uovo
Come avviene la fecondazione (?)
E manca qualcosa?✖
Grazie
Greta c’è una sezione nella pagina intitolata “quali sono i miei obiettivi (di apprendimento) per lo studio di questa unità”. La risposta alla tua domanda c’è già. se vuoi che ti risponda che gli obiettivi sono meno di quelli la risposta è “no, sono quelli”
La classe non ha capito gli argomenti, chiediamo se fosse possibile rimandare il compito, poiché nessuno si sente preparato quanto le altre volte. Speriamo prenda in considerazione la nostra richiesta.
Scusi il disturbo, cordiali saluti
La Classe 4D
Salve prof. Non so se ha ricevuto la riposta alla sua domanda da parte della classe. Comunque ci tenevamo a farle sapere che la classe non è pronta per la verifica; non perchè sia una mancanza di studio o di voglia, ma semplicemente che alcuni argomenti non li abbiamo capiti e siamo in grande difficoltà. La nostra proposta sarebbe quella di farla lunedì, dato che abbiamo due ore.
Salve prof. Sono Roberto masetti di 4A. Domani non c’è l apparato circolatorio nella verifica vero?
ragazzi i vostri commenti come vedete sono arrivati in ritardo.. abbiamo fatto lezione per due settimane su questi argomenti, avete avuto il materiale di studio completo dal 26 dicembre, potevate scrivermi per chiedere cosa non capivate, farmi domande in classe.. veramente l’8 gennaio pensate che sia giusto chiedere di rimandare il compito perchè non avete capito? comunque domani se volete potete farmi tutte le domande che ritenete. capire tutto al meglio è il nostro obiettivo, a prescindere dal compito 🙂
PS2 facebook non è uno strumento appropriato per questo genere di comunicazioni. troveremo un modo appropriato..